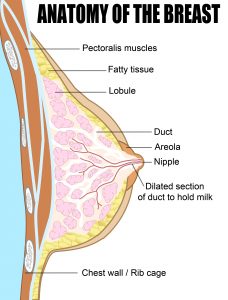
Breast – Anatomy
- Breast augmentation using implants has been an established procedure with a long historical record of safety.
- It is the most assured and quickest way to achieve the desired breast volume.
- The use of implants is one of the best breast enhancement surgery options available in Singapore.
SUITABLE CANDIDATES FOR BREAST ENHANCEMENT SURGERY
Suitable patients for breast implants include individuals with:
- Mammary hypoplasia or Micromastia (small breast)
- Significant breast asymmetry
- Slight breast ptosis
- After breastfeeding some patients experience significant upper pole breast volume loss. Suitably sized breast implant can provide some lifting effect and restoration of the upper pole volume loss.
- Post mastectomy reconstruction
PROCEDURES DONE TOGETHER WITH BREAST AUGMENTATION
- Nipple reduction
- Enlarged, drooping nipples are commonly encountered especially after breastfeeding. However, many patients often neglect the importance of a matching nipple size when considering breast augmentation.
- Nipple reduction is essential to achieve a harmonious result.
- Mommy make-over – abdominoplasty combined with breast augmentation
- It is common for women after childbirth to experience both deflation in breast volume and lax abdominal skin with stretch marks. Mommy makeover which is a combination of breast enlargement surgery (lift and implant) with abdominoplasty (tummy tuck) is a common request. This combination treatment provides significant rejuvenation effects to the entire torso.
- Mastopexy
- This is a surgery for patients with significant drooping of breast tissue. Breast implants can be inserted to provide additional volume and lifting effects.
WHAT DO I NEED TO CONSIDER WHEN UNDERGOING BREAST AUGMENTATION SURGERY?
- Here are some of the most important factors to be considered:
- Size of the Breast Implant
- Type of Breast Implant: Saline vs Silicone
- Shape of the Breast Implant
- Surface of the Breast Implant
- Surgical Incision
- Placement of the Breast Implant
- Based on Dr. Ng’s experience with Asian patients, the most common request is for teardrop shaped silicone breast implants, sized between 200-300ml placed via inframammary incision into the sub-pectoral pocket.
1. SIZE OF THE BREAST IMPLANT
- The size of the breast implant should be in proportional to body stature, height and chest circumference.
- It is also determined by the width of the breast base, the amount of breast tissue and skin elasticity.
- Placing excessively large implants will result in an unnatural appearance if there is insufficient tissue coverage.
- During the consultation, you can try a variety of implant sizes to simulate the final outcome.
2. TYPE OF BREAST IMPLANT: SALINE VS SILICONE IMPLANTS

Silicone Breast Implant – Cohesive Gel
| Saline | Silicone |
|---|
| Popularity | | |
|---|
| Texture | | |
|---|
| Shell Wrinkling | | |
|---|
| Implant Volume | | |
|---|
| Adjustment to body temperature | |
- Adjust slowly (e.g. the implant remains cold for a longer duration after a swim)
|
|---|
| Contracture Rate | | |
|---|
| Leakage |
- Leakage causes complete deflation but safely absorbable
|
- Leakage may cause local inflammation and granulomas, but much safer for modern cohesive gel implants
|
|---|
3. SHAPE OF THE BREAST IMPLANT
| Round/ Circular | Anatomical/ Teardrop |
|---|
| Profile |
- Dome shaped – less natural appearance
|
- Tear drop shape – more natural appearance
- Large variety of shapes based on different height and projections
|
|---|
| Implant Orientation | | |
|---|
| Incision |
- More options for incision
|
- Usually inframammary incision
|
|---|
4. BREAST IMPLANT – SURGICAL INCISIONS
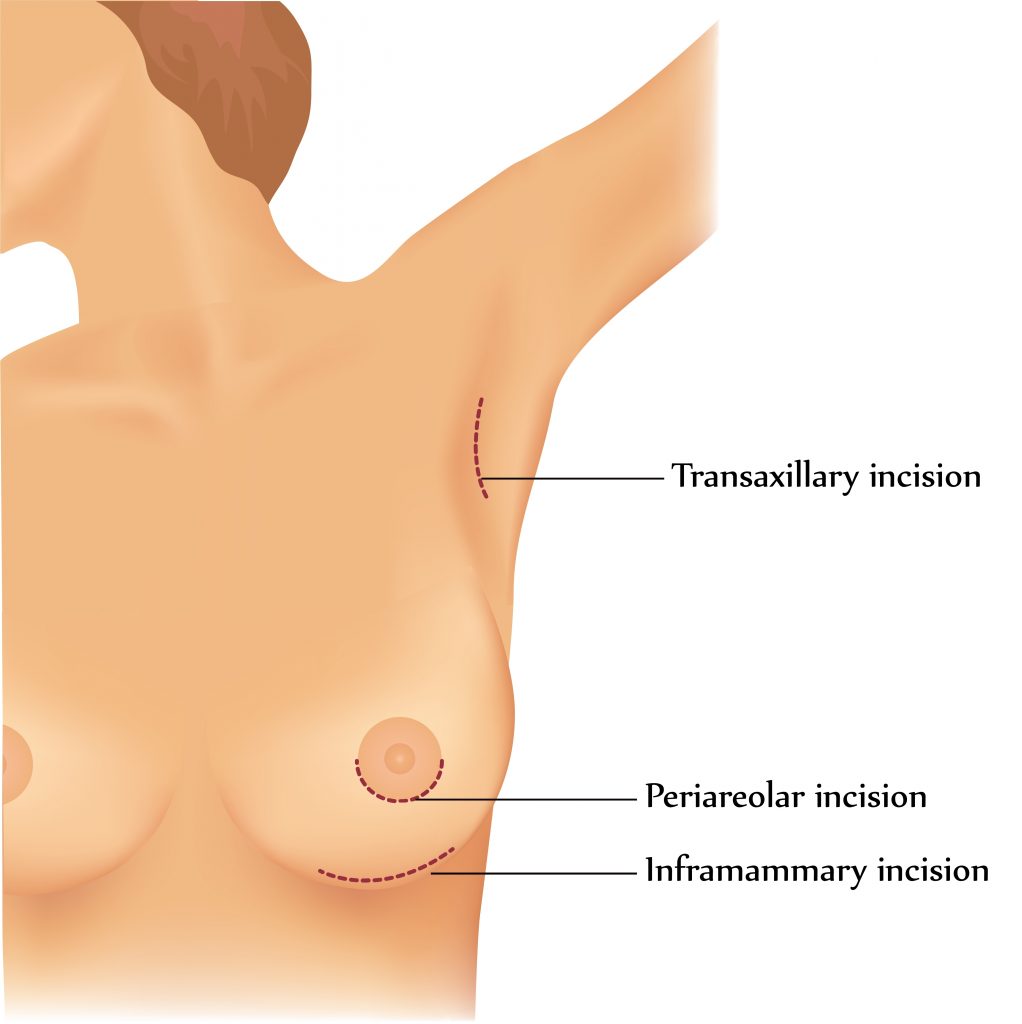
Breast implant : Choice of Incisions
| Inframammary | Periareolar | Axillary | Trans-umbilical |
|---|
| Scar |
- Scar well-hidden within breast fold
|
- Scar at areolar margin – may result in hypertrophic scars
|
- Hidden in the armpit crease but visible when wearing sleeveless
|
- Well hidden in the umbilicus
|
|---|
| Accuracy of implant placement |
- Direct visualization of orientation of implant
- Best accuracy for all implant placement
|
- Reasonably accuracy of implant placement
|
- More difficult to ascertain the orientation of implant
|
- Least accurate placement of implant
|
|---|
| Limitations on implants | |
- Limit choice of implant size if areolar diameter is < 3.5- 4 cm
|
- Difficulty with teardrop shape implant
|
- Suitable only for saline implant not for silicone implants
|
|---|
| Breastfeeding | | | | |
|---|
| Remarks |
- Most popular approach for tear drop shape silicone implant
|
- May cut through breast tissue to allow implant placement
- Risk of nipple numbness
|
- Risk of skin numbness around armpits and upper arm
- Difficult to lower inframammary fold if needed
|
- Difficult and blind dissection
- High or asymmetrical implant placement
|
|---|
5. SURFACE OF THE BREAST IMPLANT
| Textured | Smooth |
|---|
| Contracture Rates | | |
|---|
| Implant Migration | | |
|---|
| Shell Thickness | | |
|---|
Polyurethane (PU) -covered implant – had a very low contracture rate, but has been withdrawn because of a carcinogenic compound from PU breaking down (although at very low levels).
6. PLACEMENT OF THE BREAST IMPLANT
| Sub-glandular | Sub-pectoral |
|---|
| Diagram | 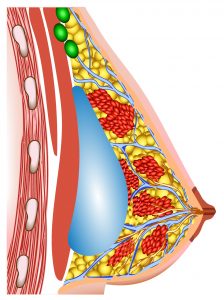 Breast implant – Sub-mammary placement | 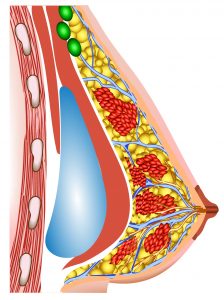 Breast implant – Sub-pectoral placement |
|---|
| Placement | Implant underneath breast tissue, above pectoris major muscle – is more anatomical | Implant underneath pectoralis muscles – is less anatomical |
|---|
| Suitable Candidates | For patient with sufficient original breast tissue – result can be very natural | For patient with very little breast tissue –pectoralis major muscle provides additional coverage to camouflage edge of implant. |
|---|
| Natural Appearance | More natural appearance if there is sufficient breast parenchymal | Better appearance for those patients with very little breast parenchymal |
|---|
| Capsular Contracture | Higher risk | Lower risk |
|---|
| Nipple Sensation | Maybe affected | Not affected |
|---|
| Implant Size Limitation | Allow larger implant | Implant size limited by size of subpectoral pocket |
|---|
| Limitation of activity | Not likely | Chest muscles contraction may cause implant to shift laterally (“dancing breast”) |
|---|
| Recovery | Slightly less pain | Slightly more pain |
|---|
- It is advisable to consult an experienced breast enlargement surgeon before proceeding with the surgery.
DESCRIPTION OF BREAST ENLARGEMENT SURGERY PROCEDURE
- Pre-operative sizing during the consultation :
- Patient to try multiple implant sizes to simulate the final outcome.
- Pre-operative screening includes a blood test and breast imaging (ultrasound, mammogram)
- In a typical surgery via inframammary incision :
- Pre-operative marking includes planning of the new inframammary fold and incision.
- Incision at the new inframammary fold
- Dissection to create space either a sub-glandular or sub-pectoral pocket for implant placement.
- Insertion of the implant.
- Meticulous wound closure in multiple layers.
- Support bra are worn immediately post-operatively.
KEY POINTS IN BREAST FILLERS SURGERY
- Accurate assessment of suitable implant size. The size of the implant has to be proportional to a patient’s body stature, height and chest circumference. It is also determined by the width of the breast base, the amount of breast tissue and skin elasticity.
- Accurate placement of the new inframammary fold.
- Most patients undergoing breast fillers surgery have insufficient breast tissue and tight skin envelope. The inframammary fold needs to be lowered to accommodate the implant to avoid a high riding appearance.
- It is crucial to determine how much the inframammary fold is to be recited according to the implant size and elasticity of the native skin envelope.
- Accurate dissection of implant pocket :
- The size of the implant pocket determines the final appearance of the implant. An inadequately dissected pocket can cause rippling of the implant surface. Over dissection can result in implant displacement and synmastia (bilateral breast pockets communicating together with loss of cleavage).
ANAESTHESIA
- Dr Ng prefers general anaesthesia for greater patient comfort and safety.
- In order to create a sub-pectoral pocket for insertion of the implant, the chest muscles need to be relaxed. This may compromise the patient’s breathing capability if done under deep sedation. General anaesthesia is safer because continuous oxygen delivery to the patient is ensured throughout the surgery.
WHAT TO EXPECT POST OPERATIVELY
- Home on the same day
- Medication includes antibiotics, pain relief and medication to reduce swelling and bruising.
- Support bra to prevent the implant from displacing laterally or riding high. The patient wears this bra for at least a month depending on the clinical outcome.
- Back to work (non-strenuous) within 2-3 days.
- Stitches (if any) are removed in about 2 weeks.
- Breast massage:
- Initiated from 2-3 weeks onwards to further improve the final appearance.
- Usually the direction of massage is downwards and inwards. This may differ depending on clinical status.
- Scar management:
- Scar massage to soften the scar
- Scar gel application to prevent scar thickening and reduce redness.
- Photo Therapy to further reduce pigmentation.
- Exercise:
- Light exercise can be restarted after 1 month.
- Avoid exercise that involved heavy usage of the pectoralis muscles for at least 2 -3 months.
- Appearance of breast:
- It is normal to expect swelling and tightness over the breast for the first 1-2 weeks. During this period of time the implant may feel more stiff and firm. The breast tissue covering the implants stretches over the next 2-3 months, the implants will feel softer and more natural.
- Final appearance is usually achieved from 3 months after the breast enlargement surgery.
RISK AND COMPLICATION OF BREAST SURGERY
- Bleeding and infection are uncommon.
- Infection is kept to a minimum by the use of antibiotics, good surgical techniques and having the surgery done in a sterile operation room.
- Synmastia
- Is a condition where both breast tissues were merged across the sternum due to over dissection during breast augmentation.
- Low risk of implant rupture due to modern day implants.
- Implant displacement
- Seroma
- Capsular contracture
COST OF BREAST AUGMENTATION
- Breast reconstruction using implant post mastectomy due to breast cancer may be considered as a non-cosmetic procedure.
FREQUENTLY ASKED QUESTIONS
Are silicone breast implants safe?
- Silicone breast implants have been used for several decades for cosmetic as well as reconstructive purpose. They have a good safety record despite being temporarily banned for cosmetic usage in the United States for possible association with connective tissue disease. This was found to be untrue and the ban was lifted.
What is the biggest implant for me?
- The size of the implant has to be proportional to the patient’s body stature, height and chest circumference. It is also determined by the width of the breast base, the amount of breast tissue and skin elasticity. The placing of excessively large implants will result in an unnatural appearance if there is insufficient tissue coverage.
What is the length of the scar?
- In most cases, the scar ranges from 3.5 to 4.5 cm depending on the size of the implant chosen. It would be unwise to place a very large implant through the narrowest incision – implant rupture during surgery rarely occurs. During the consultation Dr Ng shall illustrate this point.
- Through a very small incision, the dissection of the implant pocket and the control of bleeding (haemostasis) is much more difficult.
Can I achieve a natural cleavage after breast augmentation?
- During dissection of the implant pocket, it is conventional to keep about a 3 cm wide spacing of central chest tissue intact. This is to prevent over dissection which can result in the breast pockets from both sides communicating with each other (synmastia). This is a very difficult complication to rectify.
Do I need to replace the implants after many years?
- The silicone implant theoretically can last indefinitely i.e. the silicone in the implant does not harden over time. As long as there is no significant capsular contracture there is no need to replace the implant.
What is capsular contracture?
- The body naturally produces a thin membrane (capsule) around any implanted foreign object, this membrane normally remains thin and pliable. In some patients, significant scarring occurs in the membrane in this capsule, causing the whole construct to appear stiff and hardened (capsular contracture).
- The severity of capsular contracture has been classified by Baker (1980)
| BAKER CLASSIFICATION SYSTEM OF CAPSULAR CONTRACTURE |
|---|
| Grade I | No palpable capsule | The augmented breast feels as soft as an unoperated one. |
|---|
| Grade II | Minimal firmness | The breast is less soft and the implant can be palpated, but is not visible. |
|---|
| Grade III | Moderate firmness | The breast is harder, the implant can be palpated easily, and or implant outline (or distortion from it) is visible. |
|---|
| Grade IV | Severe contracture | The breast is hard, tender, painful, and cold. Distortion is often marked. |
|---|
| Usually implant replacement is done for grade III to IV capsular contracture. |
Can I breastfeed after breast augmentation?
- Breast enhancement surgery should not interfere with breastfeeding as long as milk ducts are not cut. Other than peri-areoalar incision there is a very low chance of affecting breastfeeding.
Can I still do breast screening examinations?
- After breast augmentation, cancer screening can still be performed using ultrasound, mammography, and MRI scan. There are special mammographic views (Eklund Displacement) available for better visualization after breast augmentation.
If you are looking to undergo breast enhancement surgery in Singapore, SWENG Plastic Aesthetic and Reconstructive Surgery is the place for you. During your consultation, Dr Ng will explain the common breast enhancement options. He will recommend the most suitable breast enhancement surgery methods used by some of the top breast enlargement surgeons, including those in Korea.
 Breast – Anatomy
Breast – Anatomy Breast implant : Choice of Incisions
Breast implant : Choice of Incisions Breast implant – Sub-mammary placement
Breast implant – Sub-mammary placement Breast implant – Sub-pectoral placement
Breast implant – Sub-pectoral placement